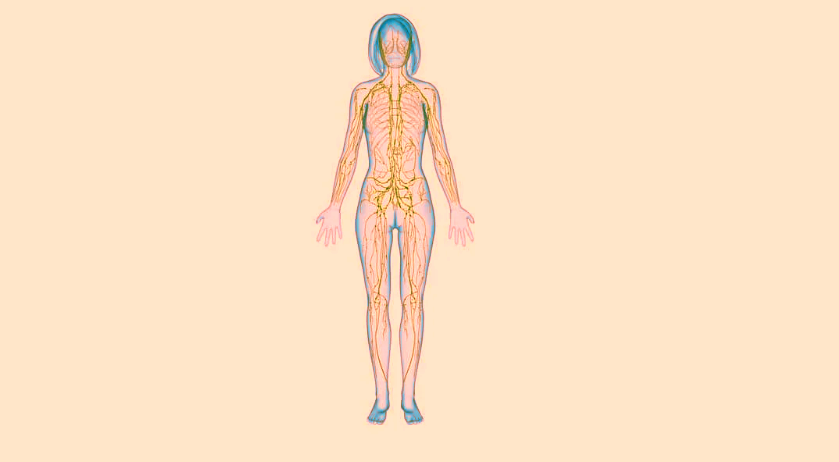
Gentle, effective treatment grounded in evidence.
ABOUT
Glasnevin MLD Clinic offers Manual Lymphatic Drainage and Combined Decongestive Therapy in a supportive and comfortable environment. Deirdre Cullivan, who runs the clinic, has over 25 years of experience as a Chartered Physiotherapist and has specialised training in the treatment of lymphatic disorders such as lymphoedema
(Vodder level III).


Deirdre:
about
Deirdre has long been amazed by the powerful effect of MLD on those she has treated. From sinusitis, to secondary lymphoedema, to acute injuries, MLD has proven itself to be an invaluable tool in her practice. Deirdre is a full member of The Irish Society of Chartered Physiotherapists, and of MLD Ireland, the professional body for therapists working in this area., and is registered with Coru. Deirdre worked for 7 years as Senior Lymphoedema Therapist at the Mater Hospital Dublin.
Deirdre is a Chartered Physiotherapist with over 25 years of experience. She has worked in a number of settings including community care and intellectual disability.



Deirdre endeavours to provide the best possible care to her patients. To this end she has attended numerous courses across different areas including a biannual review of her skills with the Vodder school. Deirdre has also completed courses in Kinesiotaping for Lymphoedema and regularly updates her knowledge with ongoing Continuing Professional Development.

Deirdre’s interest in Manual Lymphatic Drainage began when she trained as a certified manual lymphatic drainage therapist with the Vodder School in 2012. Since then she has been specialising in this area, becoming Senior Lymphoedema Therapist at the Mater Hospital Dublin in 2014, and successfully establishing her own private practice in this field.

Following cosmetic surgery such as Vaser liposuction, patients benefit substantially from the reduction in post-op swelling and bruising which comes with MLD. Deirdre has extensive experience in treating patients following Vaser liposuction, face lifts, and tummy tucks.
Lymphoedema and the lymphatic system are topics which are given little attention in the education of Health Professionals, Deirdre has a particular interest in helping others understand more about this subject. She was involved in the organisation of the first National Conference on Lymphoedema at the Mater Hospital in September 2015, and was one of the speakers at the Conference. She has lectured extensively about lymphoedema including to student Breast Care nurses and surgical teams at the Mater Hospital. Deirdre has also spoken at a NCCP Masterclass on lymphoedema in 2019, and to the Chartered Physiotherapists in Oncology and Palliative Care Special Interest group in 2020. Deirdre set up the first Early Detection of Lymphoedema Service in Ireland in the Mater Hospital in 2020, and was a Development Group member for the recently published National Lymphoedema Guidelines.





Deirdre has a special interest in helping people manage their lymphoedema themselves with appropriate compression garments, and is trained to prescribe and fit garments from a number of specialist companies, including Medi, Solidea, Juzo, and Jobst Elvarex.

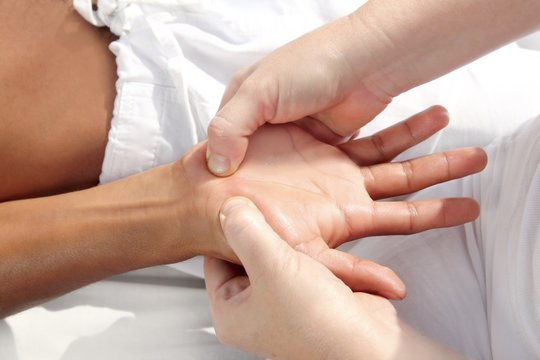

Manual Lymphatic Drainage (MLD) comprises specialised, rhythmic, and extremely gentle pumping techniques applied directly to the skin. The technique has been proven to stimulate the flow of lymphatic fluid in the body.
Manual Lymphatic Drainage is a profoundly relaxing but powerful treatment. It should only be carried out by a fully qualified practitioner who has completed specialised training in this area. MLD Ireland is the professional body of qualified therapists in Ireland.
Increased lymph flow helps the body deal with infections and damage more effectively. The movements are also known to calm the nervous system and help inhibit the passage of pain.
“Lymph Drainage is a healthy, natural, painless and absolutely effective method which gives a new basis to life, health and beauty”
Dr. Emil Vodder, 1936

These circular movements form the basis of the MLD strokes used today.
In 1929 Dr Emil Vodder and his wife Estrid, a naturopath, moved to the French Riviera and established a clinic where they started treating patients. Vodder palpated swollen lymph nodes in the cervical region in patients suffering from acne, migraines or sinus problems. He had the vision that the real cause of these pathologies was congestion in the swollen 'lymph glands', or lymph nodes as we call them today. The careful, circling, pumping movements of the skin that he developed helped to resolve the problems presented by these patients even though it was considered a taboo to work on swollen lymph nodes at the time.
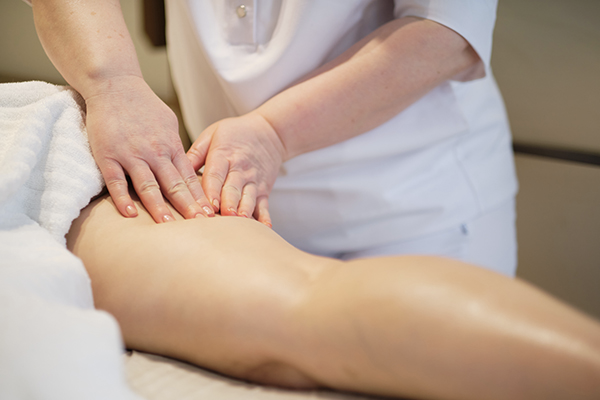

MLD has been shown to be useful in the care of patients with the following conditions:
Arm or leg oedema following treatment for breast or abdominal cancer
Primary lymphoedema
LYMPHOEDEMA RELATED TO HEAD & NECK CANCERS
SWELLING AND BRUISING POST cosmetic surgery
GENITAL LYMPHOEDEMA
venous stasis ulceration
swelling in pregnancy
digestive disorders and constipation
fibromyalgia
dermatological conditions such as acne & rosacea
chronic sinusitis
arthritic conditions
Migraines, stress headaches, etc.
MLD can also be effectively used to reduce pain and swelling following recent trauma such as:
Soft tissue injuries, especially where there's a lot of swelling and bruising
Joint replacements (especially helpful in reducing pain and swelling post knee replacement)
Recent fractures

THE LYMPHATIC
SYSTEM
This video will give you an overview of the lymphatic system. However, new research since this video was published has shown that the lymphatic system picks up 90% of the fluid which is unused by the tissues, rather than the 10% it was previously thought to carry!

See Useful Links and Articles for further information on the evidence base for MLD.

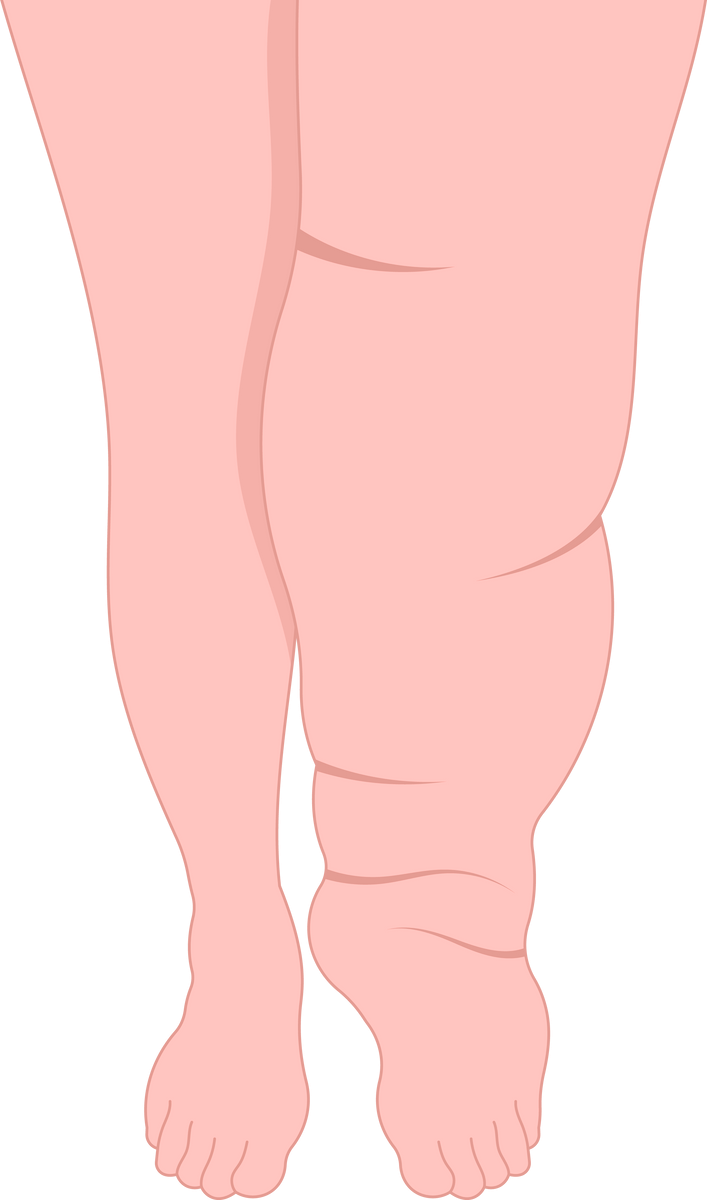
what is
lymphoedema?
Lymphoedema is an accumulation of protein-rich fluid in the tissues.
A problem with the lymphatic system can cause lymphoedema to develop in any part of the body but it mainly affects the arms or legs.
Lymphoedema may develop when lymph vessels are missing or not functioning well (Primary), or after lymph nodes are removed or damaged by radiation treatment eg. breast cancer treatment (Secondary). Left untreated, lymphedema can worsen and cause severe swelling and permanent changes, such as thickening and scarring, to the tissues of the limb.
lymphoedema
Once lymphoedema has developed there are no treatment or management miracles, but it can be managed with intervention.
how is lymphoedema treated?



0

1

When you first come for treatment the physiotherapist will carefully assess the situation and make recommendations to you about the type of treatment that may benefit you most.The treatment programme suggested will be dependent on the stage of your lymphoedema, the issues which concern you most, and the resources available to you.
Also called the subclinical or latent stage, there are no visible changes to the limb at this point, but you may notice a difference in feeling, such as a mild tingling, unusual tiredness, or slight heaviness. You can have Stage 0 lymphoedema for months or years before obvious symptoms develop.



The arm, hand, trunk, breast, or other area appears mildly swollen as the protein-rich fluid starts to accumulate. When you press the skin, a temporary small dent (or pit) forms; you may see this referred to as 'pitting oedema'. Such early-stage lymphoedema is considered reversible with treatment because the skin and tissues haven’t been permanently damaged. When you elevate the arm, for example, the swelling resolves.



When you come for an initial assessment, Deirdre will take a detailed case history asking you about any surgery/medical treatment you have had and about how your lymphoedema has developed and how it impacts on your life. She will examine you and take careful note of the condition of your limb, including skin or tissue changes and whether the oedema affects your trunk or abdomen. The limb(s) will be carefully measured and photographed to establish a baseline volume so that any changes during treatment can be noted. If necessary, Deirdre will contact your GP or Consultant to seek consent for treatment. She will outline to you the treatment regime which she feels is best for you. In the early stages of lymphoedema (Stages 0 and I) compression garments alone may be enough to manage your swelling.
In the later stages, an intensive course of Combined Decongestive Therapy (CDT) may be necessary.

3


2
This is the most advanced stage, but it is relatively rare in people with breast cancer. At stage 3, the affected limb or area of the body becomes very large and misshapen, and the skin takes on a leathery, wrinkled appearance.
The affected area is even more swollen. Elevating the arm or other area doesn’t help, and pressing on the skin does not leave a pit (non-pitting oedema). Some changes to the tissue under the skin are happening, such as inflammation, hardening, or thickening. Stage 2 lymphoedema can be managed with treatment, but any tissue damage can’t be reversed.


COMBINED DECONGESTIVE THERAPY
MLLB where layers of bandages are applied over padding to provide a compression force to the limb. This maintains the fluid reduction achieved by MLD and may result in further reduction. Deirdre usually uses a 2-layer disposable bandaging system which is easier to tolerate and less bulky.
Multi-layer lymphoedema bandaging

MLD to decongest the affected areas by opening up the lymphatic channels and diverting the fluid to areas with normal drainage.
MANUAL LYMPHATIC DRAINAGE

According to the International Society of Lymphology, Combined Decongestive Therapy (CDT), also known as Decongestive Lymphatic Therapy (DLT), is the treatment of choice for lymphoedema. This is a proven combination of treatments aimed at reducing the volume of your limb. It involves an intensive treatment phase and a maintenance phase.

EXERCISES
You will be given a programme of specific exercises to do while the bandages are in place. Bandages apply a compression force to the lymphatics and exercising in bandages augments the pumping force of the muscles.
SKIN CARE AND HYGIENE
Good skin care plays an essential part in the treatment of lymphoedema. Daily washing and application of moisturising cream will help to eliminate possible bacterial and fungal growth, and minimise the possibility of repeated attacks of cellulitis.

BREATHING EXERCISES
The thoracic duct runs upwards through the chest cavity and carries lymph back to the heart. Flow in this vessel can be improved by breathing exercises which create a suctioning effect.

Longer term follow up and support will be provided as necessary, and Deirdre is always happy to show you, or a loved one, how to bandage the limb if necessary.

The aim of treatment is to enable you to manage your condition in the longer term, to minimise the risk of complications such as cellulitis. This document is a useful resource and may be helpful to bring to your GP if you have an infection, as many doctors won’t have a great deal of expertise in dealing with lymphoedema.
The intensive phase of treatment may continue for as long as 2-4 weeks. Towards the end of this phase you will move towards the maintenance phase. You will be measured for a compression garment, either off the shelf or custom made. This garment is an essential element in maintaining the reduction in volume achieved in treatment. The garment style recommended will be carefully chosen with you to try to ensure it fits into your lifestyle so that it will be worn.


How do I go about making an appointment?
Feel free to contact us directly by email to make an appointment, or you can contact Deirdre by phone.
How long do sessions last?
Generally, a treatment session is just under an hour in length. A review appointment may be shorter.
I've just had cosmetic surgery and been advised to see Deirdre for treatment.
Will the treatment be painful?
Manual Lymphatic Drainage is a very gentle treatment and will not be painful. In fact, you should feel immediate relief from discomfort after treatment!
What should I wear for my treatment session?
It's a good idea to wear loose clothing which can be easily removed. A camisole top, or something similar, will allow easy access to the neck and shoulders which are always treated at the start of a session.
Frequently asked questions
USEFUL LINKS
& ARTICLES
-@lymphmadesimple on Instagram: follow our page for common myths, questions, and concerns, as well as community engagement
Here are some useful resources to learn more about lymphoedema and related concerns:

FeES
Manual Lymphatic Drainage................................................€100
Combined Decongestive Therapy.........................................€100
-Fees are per session, lasting approx. 1 hour
-Additional costs will apply to bandages
-A cancellation fee of €20 applies in most cases where less than 24 hours' notice is given
Visits to Chartered Physiotherapists are covered by all leading health insurers, including VHI, Hibernian Aviva, Quinn, ESB Medical, Garda Medical, and HSF.
You may be able to claim tax relief on Physiotherapy costs by submitting a Med1 form to Revenue.
REDUCING
YOUR COSTS



For more information or
to make an appointment,
please reach out
by email here: